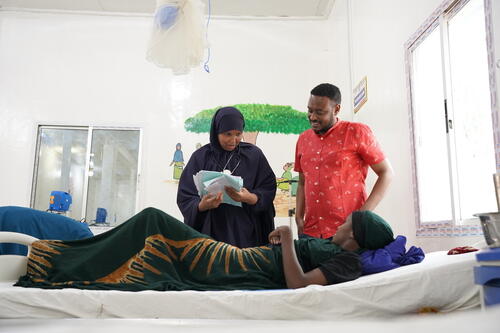
When Aisha* began haemorrhaging, experiencing heavy, potentially life-threatening bleeding, just ten days after giving birth to twins at home in Diinsoor district, in the Bay region of Somalia, her family feared the worst. The hospital where she had safely delivered her previous children was no longer operational. With limited healthcare available in their community, her husband urgently borrowed money and drove five hours through the night to reach Bay Regional hospital in Baidoa, one of the few facilities offering free, quality maternal and paediatric care, and where Médecins Sans Frontières (MSF) works. Medical teams quickly stabilised Aisha, successfully treating her severe bleeding.
Limited access to healthcare leads to patients arriving at hospitals with severe complications, sometimes resulting in preventable maternal and neonatal deaths. Insecurity, scarce healthcare services, and logistical challenges further hinder access to timely care. Cultural norms, such as requiring male consent for surgical interventions, add critical delays when immediate action is necessary.
Stories like Aisha’s are all too common across Somalia’s Southwest state, where women and children often travel hundreds of kilometres to seek lifesaving medical care. Those unable to afford the journey face severe consequences.
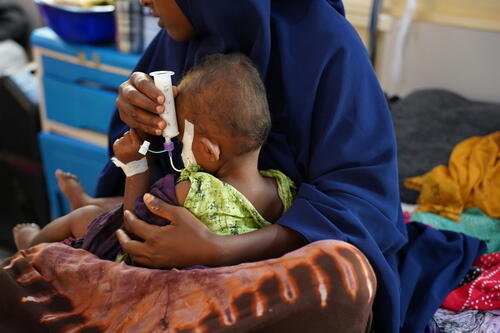
Hawa, an 18-year-old mother of two, delivered her first child at age 16 at home with only relatives present. “We don't have hospitals or doctors nearby,” she says. After her second childbirth, she experienced serious complications, including swelling and cardiac issues. Determined, she travelled to Baidoa for treatment. Now recovering, Hawa voices a widespread hope: “We need a hospital in our area and doctors who can come to us.”
Multiple factors hinder people’s access to care. Poverty, insecurity, distance, and cultural barriers all significantly delay treatment. Hassan, a 28-year-old father from Afurow village, tragically lost his wife during childbirth at home due to the absence of health facilities and skilled birth attendants. Left alone with a newborn son who soon fell critically ill, Hassan struggled.
“He had diarrhoea and vomiting,” says Hassan. “Medicines from local pharmacies didn’t help.” After two months of deteriorating health, he learned of MSF’s free services in Baidoa. “I borrowed about US$130 and travelled 150 kilometres to reach the hospital,” he explains. What began as a desperate situation has turned into hope, as his son receives essential treatment and nutrition care.
Medicines from local pharmacies didn’t help. I borrowed about US$130 and travelled 150 kilometres to reach the hospital.Hassan, father of a patient at Bay Regional hospital
MSF has been supporting Bay Regional hospital since 2017, providing emergency obstetric, neonatal, paediatric, and nutrition care. In 2024 alone, MSF treated over 14,000 children for malnutrition, conducted more than 38,000 paediatric consultations, assisted in over 2,800 births, and carried out approximately 35,000 reproductive health consultations, all free of charge. Yet despite these efforts, the region’s maternal and child health situation remains critical, especially after recent funding cuts
The suspension of USAID funding has led to the closure of at least 37 health and nutrition sites in both rural and urban areas around Baidoa. Consequently, patient numbers at remaining facilities like Bay Regional hospital have surged, overwhelming an already fragile healthcare system.
From January to June 2025, MSF teams at Bay Regional hospital treated 11,894 malnourished children, an increase of 76 per cent compared to the same period last year. This significant surge in malnutrition admissions, along with rising cases of maternal health complications, underscores the urgent need for sustainable and efficient funding to restore and expand essential services, especially in underserved rural communities.
Families frequently delay seeking medical assistance until conditions worsen, often relying initially on traditional healers. Misconceptions surrounding vaccinations, such as beliefs linking them to infertility or other illnesses, further limit access to preventive care. Continuous health education and community engagement are essential to building trust in medical services and encouraging timely care-seeking.
“Maternal and neonatal deaths can be prevented by ensuring pregnant women have timely access to care closer to home,” says Dr Pitchou Kayembe, head of MSF’s programmes in Somalia. “Too often, patients reach us in critical condition simply because healthcare isn’t available nearby.”
Dr Kayembe emphasises that while MSF continues delivering lifesaving care, broader systemic support is vital.
“The scale of the need demands sustained, long-term investment and strategic support across Somalia,” he says. “We urge donors and humanitarian partners to prioritise expanding general and emergency maternal and paediatric healthcare, particularly in remote areas.”
Inside Bay Regional hospital’s busy wards, newborns take their first breaths under skilled supervision, malnourished children gradually regain health, and frightened mothers find relief and hope. As Dr Kayembe concludes, “It’s not just about responding to immediate crises. It’s about ensuring families survive, recover, and rebuild their lives starting with dignified, quality healthcare for all.”
For over four decades, Médecins Sans Frontières (MSF) teams have been providing medical and humanitarian care to the Somali people across the Horn of Africa. In Somalia, MSF continues to respond to the medical needs of people displaced by ongoing conflict and extreme weather events, and to support services in Ministry of Health facilities. A significant part of our work focuses on offering specialised training for healthcare staff, improving the quality of healthcare, rehabilitating hospitals, enhancing water, sanitation and hygiene services, and conducting health education sessions to ensure infection prevention and control in health facilities. MSF is currently running medical activities in three locations; Baidoa, Bay region (Southwest state), and in Galkayo North (Puntland state), and Galkayo South (Galmudug state).
*Patient name was changed to protect privacy.