In September 2025, Médecins Sans Frontières (MSF) concluded our project in Cross River state, Nigeria, after three years of collaboration with the state ministry of health. We provided free, comprehensive healthcare to thousands of people living in Akor and Old Ndibeji, located in Akampa local government area, near the Nigeria-Cameroon border. Launched in May 2022, the project supported two basic healthcare centres in communities whose access to medical services had been extremely limited. After donating medical supplies, MSF handed over operations to the Ministry of Health (MoH).
For many community members like Achifone Felix, MSF’s presence was the difference between life and death.
“MSF has helped me survive,” says Felix. “I am a patient with high blood pressure, and when I came here during my retirement, MSF attended to me and provided free medication. Without their support, many of us would not be alive today.”
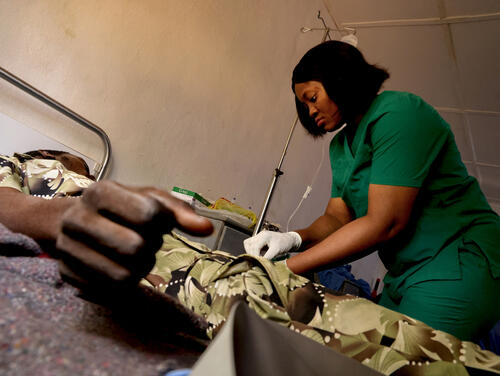
A lifeline for remote communities
During our three-year presence, MSF became a lifeline for remote communities. Working alongside incentivised MoH staff, our teams conducted more than 73,000 outpatient consultations, admitted over 8,000 patients for observation before referring them for further treatment in Calabar, and supported 2,123 deliveries. They also provided 3,887 antenatal consultations, 5,776 family planning sessions, and administered 9,303 vaccinations.
Malaria, endemic in the region, was the leading cause of illness among the patients we cared for, with nearly 30,000 cases treated. People also received care for other common conditions including injuries, respiratory infections, and typhoid fever.
Training and capacity building
Beyond patient care, we also provided training for local staff as an investment in the sustainability of healthcare services in this part of Cross River state.
When we started in 2022, the need was overwhelming. People had to travel for hours to get basic care. Today, looking back at the thousands of consultations, deliveries and lives saved, it’s clear this project made a real difference.Meria Nadje, MSF project coordinator
“When I finished school, I had no experience in patient consultation,” explains Owen Helen, a Ministry of Health nurse working with MSF. “But after joining MSF, and spending three years with them, I gained the skills to manage patients confidently.”
“Now I know how to consult, perform procedures like circumcision, and provide family planning services — all of which I learned while working with MSF,” he says. “Today, I can carry out these tasks independently and effectively.”
Emergency care and long journeys
The facilities offered basic emergency obstetric and newborn care, ensuring essential and safe care for pregnant women, mothers and newborns during childbirth. On average, MSF teams managed 54 deliveries each month, and referred between 20 and 40 women with pregnancy complications to tertiary hospitals in Calabar, the state capital.
During the rainy season, this route took roughly eight to 10 – sometimes up to 12 – hours to travel. Other times, the road would be washed out completely, delaying transport further. Referrals were mostly for paediatric cases, complicated sexual and reproductive health issues, severe malaria, injuries, and surgical complications. MSF covered all costs for referred patients, including medical bills, transport and food.

“My uncle fell seriously ill in the middle of the night, and we rushed him to the MSF facility here in Old Ndibeji,” says Alhaji Abdulwahab Achigi, a resident of Old Ndibeji. “The nurses worked tirelessly to stabilise him, and by morning he was already better. He was admitted free of charge, and the medicines were also free. Later, they arranged to transfer him to the teaching hospital in Calabar.”
Community-based approach
The project adopted a community health model, reaching 17 communities through house-to-house health promotion, a referral system to higher-level care, and follow-up care in the community. This approach helped bridge gaps in health awareness and encouraged timely care-seeking.
Challenges and achievements
Operating in these remote communities posed significant challenges, from long distances to seasonal disruptions to the roads, hindering medical transfers. Despite these obstacles, MSF ensured free, quality care and lifesaving support for thousands of people who otherwise had little access to health services.
“When we started in 2022, the need was overwhelming,” says Meria Nadje, MSF project coordinator. “People had to travel for hours to get basic care. Today, looking back at the thousands of consultations, deliveries and lives saved, it’s clear this project made a real difference.”






